Glaucoma Treatment in Portland OR
What is glaucoma?
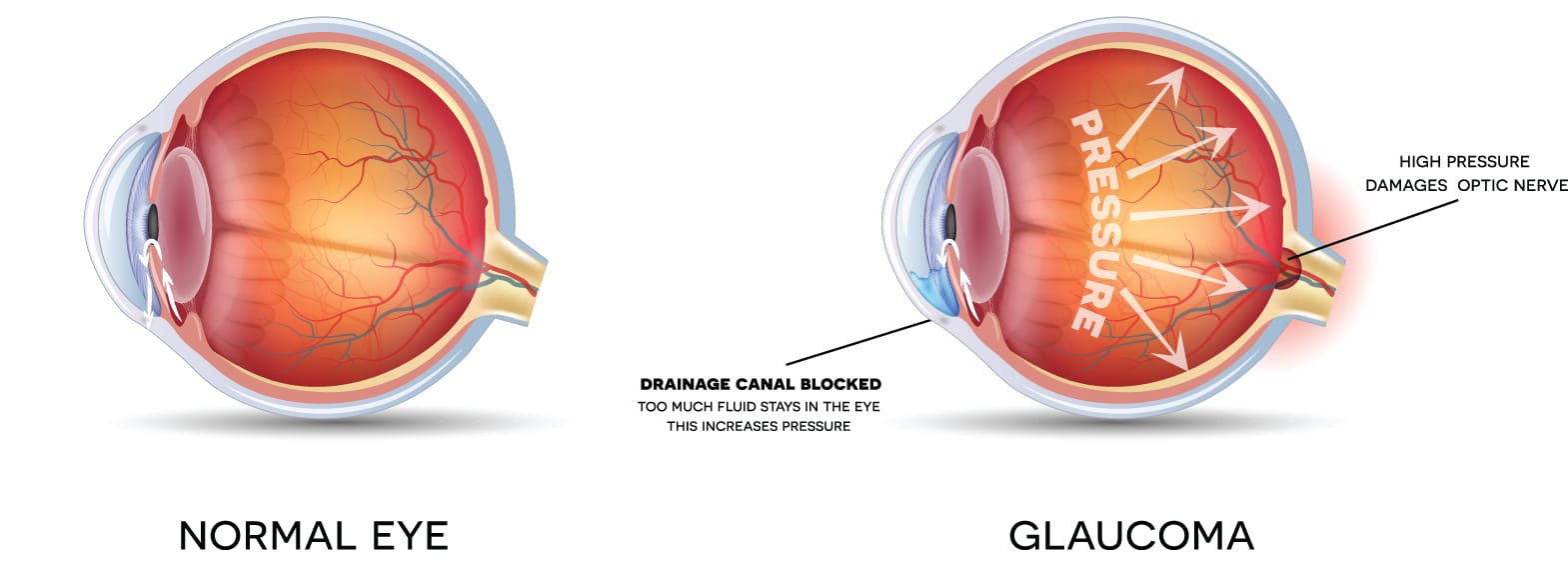
Glaucoma is a group of eye conditions where pressure builds inside the eye, and this increased pressure damages the optic nerve. It is second only to macular degeneration for blindness across all age groups in the U.S. Glaucoma is especially dangerous because many forms have no warning signs — before the patient realizes there is a problem with his or her vision, damage has already occurred. This damage is permanent.
What causes glaucoma?
A substance known as aqueous humor flows through a normal eye and exits through an area of tissue called the trabecular meshwork. The trabecular network is found where the iris and cornea meet. If the trabecular meshwork has a blockage or is somehow damaged, or when the eye overproduces aqueous humor, pressure increases inside the eye. As the pressure increases and stays elevated this damages the optic nerve. As the nerve gradually deteriorates blind spots develop in the patient’s visual field.
Who Is at risk for developing glaucoma?
Anyone can develop glaucoma, but certain factors increase a person’s risk:
- Having high intraocular pressure
- Being over age 60
- Being black, Asian, or Hispanic
- Having a family history of glaucoma
- Having other medical conditions, such as diabetes, high blood pressure, heart disease, or sickle cell anemia
- Having corneas that are thin in the center
- Being extremely nearsighted or farsighted
- Having had an eye injury
- Having had certain types of eye surgery
- Long-time use of corticosteroid medications, particularly eye drops
Symptoms of glaucoma
While there are different forms of glaucoma, the two most common forms are known as open-angle glaucoma and acute angle-closure glaucoma. These are the symptoms for these forms:
Primary open-angle glaucoma symptoms:
- Patchy blind spots in your peripheral or central vision, frequently in both eyes
- Tunnel vision with advanced glaucoma
Acute angle-closure glaucoma symptoms:
- Severe headaches
- Eye pain
- Nausea and vomiting
- Blurred vision
- Halos around lights
- Eye redness
Is Glaucoma Hereditary?
Primary open-angle glaucoma, the more common type of glaucoma, is hereditary. This means that if you have an immediate family member who has glaucoma, you are at a higher risk and are more likely to develop glaucoma at some point in your life.
Early-onset glaucoma also tends to be hereditary, so those with a family history of glaucoma should make sure to get regular eye exams before the age of 40.
Can My Sight Be Restored If It Was Lost Due to Glaucoma?

Glaucoma treatments are effective at preventing and slowing potential vision loss, but there is no known treatment to reverse the damage caused by glaucoma. Any vision you have lost cannot be restored, which is why an early diagnosis is crucial to preserving your eye function.
Importance of Eye Exams for Glaucoma Prevention and Treatment
Regular eye exams can be the difference between saving your vision and losing it permanently. As you develop glaucoma, you may not notice any symptoms, so only a comprehensive eye exam will catch the changes and the buildup of pressure in your eye.
Catching glaucoma early, when it can more easily be treated, will maximize your chances of preserving your eyesight and preventing irreversible damage before it becomes too late.
How Often Should You Visit Your Eye Doctor for Glaucoma?
In order to prevent and catch glaucoma early in its development, you should see your eye doctor for regular visits to check your eye health and track any changes in your vision.
As you get older, your risk for developing glaucoma increases, so it is recommended that those over 40 have their eyes checked every two to four years and those over 60 be checked at least once a year.
For those already diagnosed with glaucoma, we recommend ongoing follow-up visits to continually check for new or worsening developments. Depending on the type and stage of your glaucoma, you may need to visit your eye doctor anywhere from one to four times a year, with more severe cases requiring more frequent check-ups.
Diagnosing Glaucoma
While some patients may experience symptoms from glaucoma as the disease progresses, others do not learn they have the condition until they undergo a routine eye exam. There are several different exams performed to diagnose glaucoma, including a visual field and visual acuity test. These tests measure peripheral vision and how well patients can see at various distances. Other tests may also be performed, such as tonometry to measure the pressure inside the eye and pachymetry to measure the thickness of the cornea.
Glaucoma Treatment Options
Once we’ve diagnosed a patient’s glaucoma, it’s important to quickly begin lowering the pressure in inside the eye caused by the buildup of fluid. The goal is to prevent additional vision damage.
The first treatment option is prescription eye drops. Beyond that, surgery may be necessary to improve fluid drainage. Your doctor will recommend a treatment option based on your needs including:
- Eye drops — There are now a variety of different eye drop options for glaucoma treatment, depending on how your eyes respond. Some of these eye drops increase outflow of the aqueous fluid. Others seek to reduce production of fluid in the eye. Many people don’t comply with their dosages and the need for consistent application of their eye drops. This is the leading cause of continued damage to the optic nerve. This lack of urgency can be attributed to the fact that that the patient isn’t experiencing any pain or symptoms.
- Surgery — With surgery the goal is to improve fluid drainage within the eye.
- Laser therapy: There are three options for laser surgery for glaucoma: laser trabeculoplasty, iridotomy, and cyclophotocoagulation. These procedures seek to increase outflow of fluid in the eye or to eliminate blockages in the trabecular meshwork.
- Filtering: In a trabeculectomy, part of the trabecular meshwork is removed to enhance drainage.
- Drainage tubes: Small tubes are inserted, usually through the trabecular meshwork, to open flow.
- Minimally invasive glaucoma surgery: These various techniques are used to lower eye pressure, generally with lower risk and easier recovery.
Glaucoma Patient Testimonials
How to prevent glaucoma
While there are no surefire ways to prevent glaucoma from developing, regular screenings and early detection are the best forms of protection against the harmful damage that the disease can cause. Patients should have a comprehensive dilated eye exam at least once every two years, especially if they have a higher risk of developing glaucoma. Older patients may be encouraged to be tested more frequently.
Click here for additional information on Glaucoma »
are there permanent treatment options?
Glaucoma can be prevented, but there isn’t a cure once it develops. Damage to the optic nerve is permanent. Once glaucoma is diagnosed, however, treatment can help slow or prevent vision loss, but this can only happen with an early diagnosis. That’s why we stress the importance of regular eye exams at The Eye Clinic. Once diagnosed, the goal is to lower the intraocular pressure.
Learn more about the causes and treatment of glaucoma in Portland, OR by filling out the contact form below!
Schedule a Glaucoma Consultation!
To learn more about Glaucoma or the various treatments The Eye Care Clinic offers, or to determine whether you are a candidate for treatment, schedule a consultation with one of our top doctors today! Call (503) 297-4718 or fill out the Consultation Request Form below, and our staff will help you arrange your appointment. Our practice serves Portland and the surrounding Oregon areas, and we look forward meeting you!