Uveitis Treatment in Portland, OR
If you are suffering with irritation or swelling in your eyes, you may be suffering from Uveitis. At The Eye Clinic P.C., our experienced doctors offer personalized treatment for patients in Portland and the surrounding areas. Call (503) 297-4718 today to learn more or to schedule a consultation for treatment!
“A happy place where people really care about your eyes and eyesight. Nice pleasant environment, friendly staff, Been going there for years (50) and have received the best service possible. – T.B.
What is Uveitis?
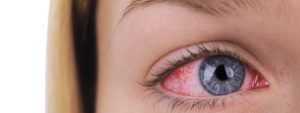
Uveitis is an irritation and swelling of the uvea, which is the highly vascular fibrous tissue that forms the iris, choroid, ciliary body, and pars plana. It can be caused by autoimmune disorders, infections or foreign toxins, but often the cause is unknown. It frequently manifests in young to middle-aged individuals and may only affect one eye.
What Are the Different Types of Uveitis?
Uveitis is generally classified based on the part of the eye where inflammation is present. Different types include:
- Anterior. The most common type of uveitis, anterior uveitis involves inflammation at the front of the eye. Signs of anterior uveitis tend to occur suddenly and, if mild, may resolve spontaneously. Still, it is important to see a specialist for a full evaluation. Anterior uveitis can also come and go, requiring ongoing management.
- Intermediate. This type of uveitis, characterized by inflammation in the middle area of the eye, is more common in young adults. The middle of the eye is where vitreous fluid fills the center of the eye globe (eyeball). Intermediate uveitis can also go away and come back or get worse over time.
- Posterior. A type of uveitis that affects the inner part of the eye, posterior uveitis is not very common. It causes the most severe and concerning symptoms due to its proximity to the retina, optic nerve, and the choroid, the blood vessels that deliver blood to the retina. In posterior uveitis, symptoms may recur and last for many months at a time.
- Panuveitis is the rarest form of this inflammatory disease, and also the most severe in terms of risks to vision. In panuveitis, inflammation is present in all three layers of the eye.
What causes uveitis?
In about half the cases of uveitis, a specific cause can’t be pinpointed. But in the other half, these are the usual causes:
- Eye injury
- Eye surgery
- Autoimmune disorder, such as ankylosing spondylitis
- Inflammatory disorder, such as Crohn’s disease or ulcerative colitis
- Infection, such as Lyme disease, herpes zoster, West Nile virus, etc.
- Cancer that affects the eye, such as lymphoma
How common is Uveitis?
Uveitis is categorized as a rare disease. It seems to occur in fewer than 40 in 100,000 people in the United States. However, statistics also indicate that nearly 30,000 cases of vision loss are attributed to uveitis each year. The condition can affect children as well as adults and is diagnosed in smokers more often than in people who do not smoke.
What Are The Symptoms Of Uveitis?
The symptoms usually develop quite quickly and unexpectedly, but in some individuals they form slowly. Distinguishing symptoms of uveitis may include:
- Irritation and redness of the eye
- Eye pain
- Sensitivity to light
- Dark floaters and blurred vision
This may affect the front of the uvea (iritis), the back of the uvea, the middle (the vitreous) or the entire span of tissue.
Who is at Risk For Developing Uveitis?
Patients with rheumatoid arthritis, AIDS, herpes syphilis and direct eye trauma have a higher risk for developing uveitis. If the disorder is not treated, permanent vision loss may result due to damage to the optic nerve. Additionally, there may be an increased risk of cataracts and glaucoma due to the eye’s weakened condition.
What happens if my Uveitis goes untreated?
Uveitis can be a serious condition that leads to swelling in the retina, scarring of the retinal tissue, cataracts, glaucoma, and damage to the optic nerve. It can cause retinal detachment and carries a risk of permanent vision loss. If you exhibit the signs of uveitis, it is essential that you consult with a specialist who is familiar with the diagnosis and treatment of this disease.
How is uveitis diagnosed?
If you’re experiencing any of the symptoms of uveitis, such as pain, redness, sensitivity to light, and new floaters, we need to see you at The Eye Clinic. When diagnosing uveitis, Dr. Wilkins and Dr. Donohue will conduct a complete eye exam, plus they’ll go through your health history. This is important to show autoimmune conditions that could be behind your uveitis inflammation.
We may also use additional tests to confirm our diagnosis:
- Blood tests
- Analysis of the fluid from the eye
- Photograph that evaluates the retinal blood flow (angiography)
- Photography to measure the thickness of the retinal tissues and to determine the presence or absence of fluid in or under the retina
How can I prepare for Uveitis treatment?
Uveitis Treatment
There are several treatments for uveitis depending on what part of the eye is affected and how severely. In some cases, the underlying condition (herpes, AIDS, syphilis) may need to be treated to see improvements in the uveitis. Otherwise, the patient will be encouraged to wear dark glasses and take pupil dilating drops to relieve pain and pressure. Serious cases usually require extended use of steroid eye drops as well as oral steroids that suppress the immune system. Click here for additional information on Uveitis
See What Our Patients Are Saying!
“My experience at The Eye Clinic is always positive from the time I walk it. Check in is handled quickly; and care is provided on a timely basis. Dr Wilkins is the best! All the staff are cordial and strive to make one comfortable.” – L.S.
What is recovery like from uveitis?
Depending on the type and severity of uveitis, patients may see improvement in as little as two to five weeks after beginning an appropriate treatment plan for their inflammation. Sometimes, though, it can take months for symptoms to resolve completely. It is important to receive care right away when the signs of uveitis develop. Early diagnosis and treatment could accelerate the recovery from the condition.
What can I expect from my results?
When treated early, uveitis tends to come under control quite well. Some patients whose vision has been disrupted by the inflammation may regain better visual clarity as the condition subsides. Depending on the type and severity of the disease, it may be necessary to continue a treatment protocol for many months or years. Doing so can slow or stop the progression of the disease and manage risks to the retina and optic nerve.
Can uveitis recur?
Yes. Again, that shows the importance of continuing eye exams on a yearly basis if you’re over 50. That way if uveitis returns, we can treat it again.
Can you prevent uveitis?
There isn’t any particular method or behavior that can prevent uveitis. Of course, this is completely the case in the roughly 50 percent of people where the cause cannot be pinpointed. Seeking proper treatment for an autoimmune disease or infection is the best method for preventing uveitis. Smoking is thought to play a role, as well.
What’s most important is to keep your regular eye exams with Dr. Wilkins and our team at The Eye Clinic, as early detection and treatment are important to reduce your risk of vision loss.
Can uveitis cause blindness?
Yes. Uveitis causes about 30,000 new cases of blindness in the United States every year. Uveitis may cause blurry and reduced vision. When treated, vision may recover. In some cases, mostly in intermediate uveitis, posterior uveitis, and panuveitis, where inflammation is recurrent and chronic, damage to the eye can occur, particular to the retina and optic nerve. This causes permanent vision loss.
Inflammation caused by uveitis can cause pressure inside the eye to rise. This is glaucoma, and it can damage the optic nerve creating permanent vision loss.
Cystoid macular edema is a complication usually seen with intermediate uveitis, posterior uveitis, and panuveitis. This is swelling of the macular, the most sensitive part of the eye necessary for driving, reading, and detailed up-close work. If swelling doesn’t respond to treatment, the sensitive cells under the fluid can die and cause vision loss.
Another complication of uveitis is damage to the vitreous, the clear gel-like substance that fills the eye. Inflammation from uveitis can allow debris to get into the vitreous. This may be blood and scar tissue and it can cause floaters or flashes of light. It may even block vision. A vitrectomy could then be required to replace the vitreous with a clear fluid.
Uveitis can also increase the risk of a detached retina, which requires immediate surgery to prevent blindness.
Does Stress Cause Uveitis?
While underlying health conditions and physical trauma to the eye are typically the causes of uveitis, it is true that stress, lack of sleep, and anxiety can worsen the symptoms of uveitis. Although there is no direct correlation between stress and uveitis, it’s important that patients manage stress levels and establish an adequate sleep routine to prevent worsening symptoms. Uveitis can happen once your immune system is at work fighting an infection, or what it thinks is an infection, in the tissues of your eyes. By getting enough sleep, your body will repair itself and its immune system to lessen the pain and other symptoms caused by uveitis.
What Percentage of Patients with Uveitis Go Blind?
35% percent of patients who suffer from Uveitis experience visual impairment, loss of vision, or partial blindness. However, only 10% – 15% of these patients experience total blindness caused by uveitis while suffering from other eye conditions such as cataracts or glaucoma, which can speed up the process of losing your vision faster. Leaving your uveitis untreated may cause chronic eye pain or blindness. If you’re experiencing any of the uveitis symptoms listed above, contact The Eye Clinic in Portland, OR.
Will My Vision Get Restored After Uveitis Treatment?
After the use of recommended treatment, many patients are able to fully recover from uveitis, and their vision is often restored back to normal, along with the elimination of eye pain, redness, and other symptoms. However, if you suffer from intermediate uveitis or posterior uveitis, permanent damage to your vision may have occurred and may require further treatment if you are looking to completely restore your vision.
While dark glasses and eye drops can help improve symptoms, eliminating uveitis can take some time. Most patients begin seeing improvements in their vision and symptoms within two to five weeks. For those with more serious cases of uveitis, it may take several months to heal. Regardless, treating uveitis can be a life-changing experience as many patients can begin to see without experiencing pain.
Call The Eye Clinic P.C. For Uveitis Treatment!
Interested in learning more about treatment for Uveitis? Call us at 503.297.4718 or submit an online contact form with our Portland ophthalmologists today! Our practice serve Portland and the surrounding areas of Oregon.